REFORM prints a 3D model based on a VOXEL-BY-VOXEL framework
Import 3D models in ‘.stl’ format, adjust the filament extrusion rate per voxel, and specify different mechanical properties for your 3D printed objects.
THE FIRST IMAGE-GUIDED SLICING SOFTWARE FOR 3D PRINTERS
We have developed a new slicing software named ‘REFORM’ for advanced applications utilizing Fused Filament Fabrication (FFF) technology.
Explore our collection of tutorials on our YouTube channel, designed to provide helpful guidance and tips for navigating REFORM.
We continuously experiment with the latest updates in the field of 3D printing technology and conduct research and fabrication of new materials.
Morphé is currently working on its own 3D printer featuring a unique rotatable extruder with three different hot-ends.
REFORM prints a 3D model based on a VOXEL-BY-VOXEL framework
Import 3D models in ‘.stl’ format, adjust the filament extrusion rate per voxel, and specify different mechanical properties for your 3D printed objects.

REFORM is an image-guided slicing software designed to generate geometric code (g-code) for material extrusion-based additive manufacturing (MEX-AM), commonly referred to as fused deposition modeling (FDM) or fused filament fabrication (FFF). In contrast to conventional slicing software, REFORM adopts a novel volumetric approach, utilizing volumetric slices determined by grayscale images at specified layer heights. REFORM’s g-code generation is characterized by a unique feature— it introduces an additional parameter for manipulating extrusion flow, printing speed in a voxel-based framework.
.
The term ‘infill pattern’ denotes the internal structure of a 3D printed object. It can range from simple linear patterns to more intricate designs, affecting factors such as the object’s strength, flexibility, weight, and printing time. With ‘REFORM’ slicing software, users have the ability to customize their own patterns to suit their specific requirements. This includes creating patterns with varying filament extrusion rates or selecting from a range of pre-designed options.

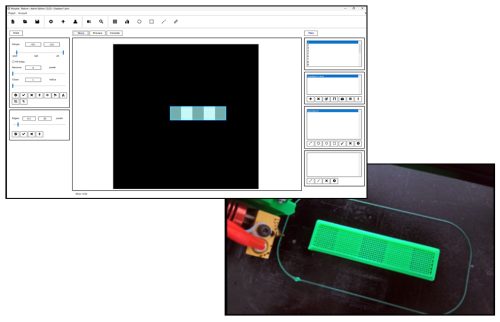
The filament extrusion rate determines the quantity of melted filament to be extruded during printing. By precisely adjusting the extrusion rate and printing speed throughout the 3D printing process, it becomes feasible to modify the final properties of the 3D printed object. Import 3D models and vary the filament extrusion rates for each print, yielding parts with diverse characteristics such as weight, flexibility, strength, or other properties dependent on the chosen filament.
PRINT DIRECTLY FROM IMAGES
REFORM connects images directly to the printing process, allowing users to produce 3D printed objects from various image formats such as DICOM, BMP, JPG, TIFF, etc., eliminating the need for 3D models. This results in outcomes with high internal accuracy.
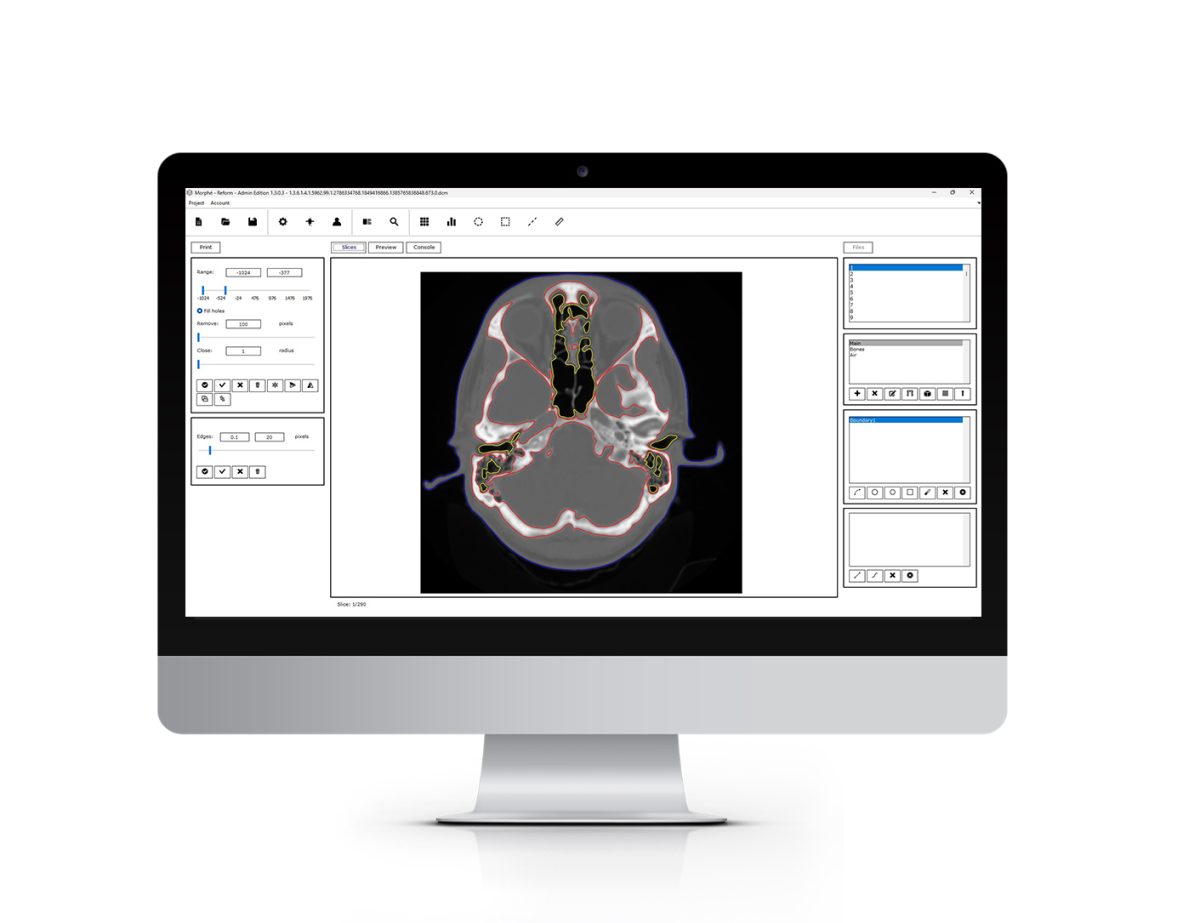
Morphé’s new slicing software named ‘REFORM’ can connect medical images in DICOM or any other format directly to the printing process. REFORM handles image segmentation, g-code production, and the printing process, enabling users to create 3D printed solutions without the need for 3D models. This leads to personalized outcomes with high accuracy.
The results from the use of ‘REFORM’ indicate higher control of the extrusion flow based on a patient’s anatomy compared to the existing methods and available slicing software. The innovative approach could reduce lengthy pre-processing times and simplify the production of 3D printed anatomical models.

Learn more about our projects, gain insights, share your creativity.
PARTNER
EDITION IS NOW AVAILABLE!
LIFETIME – Access to all up-coming updates of the professional REFORM 1.XX version and print directly from images such as DICOM, bmp, jpg, etc.
TECHNICAL SUPPORT – The Morphé team is here to HELP and guide you through any issues via our community forum, emails, and video meetings.
READY-TO-USE – Download and start using REFORM immediately after your purchase.
SUPPORTING US – You are supporting the team of MORPHE in their ongoing work to improve the current slicing tools, and develop new ones.
Explore our collection of tutorials on our YouTube channel, designed to provide helpful guidance and tips for navigating REFORM. Whether you’re just starting out or looking to refine your skills, this is the best way to begin. Join us as we share our knowledge and expertise, helping you overcome challenges and achieve your printing goals. Subscribe today to stay updated and take your printing skills to the next level.

Achieve results of high accuracy using our software and prototype 3D printer with a rotatable triple-head extruder.

This extruder allows the use of three different types of filaments, as well as, the use of a diffenet nozzle diameter per a hot-end. Despite the fact that REFORM allows the manipulation of the extrusion rate of all the hot-ends able to be used at the same layer; the software provides the maximum perfromance, when is connected to our 3D printer.
Morphé, led by a group of young engineers, has developed the FIRST image-guided slicing software for extrusion-based 3D printers called ‘REFORM’. Our goal is to make this technology accessible to everyone by providing accurate and personalized solutions.
Okkalidis, F., Chatzigeorgiou, C., Okkalidis, N., Dukov, N., Milev, M., Bliznakov, Z., Mettivier, G., Russo, P. and Bliznakova, K.
Technologies, 12(8), p.139.
https://dx.doi.org/10.2139/ssrn.4601778
This paper presents characterization of seven novel materials for material extrusion-based additive manufacturing (MEX-AM) and twenty-two commercially available filaments, in terms of x-ray Computed Tomography (CT) numbers, as tissue mimicking materials for the realization of 3D printed organ body phantoms. Two approaches, by 3D printing of cube samples and by producing cylinders of melted materials, are used in achieving the goal. Results showed that the CT numbers, given in Hounsfield Unit (HU), of all the samples depended on the beam kilovoltage (kV). The CT numbers ranged from +411 HU to +3071 HU (at 80 kV), from -422 HU to +3071 HU (at 100 kV), and from -442 HU to +3070 HU (at 120 kV). Several commercial and custom-made filaments demonstrated suitability for substituting soft and hard human tissues, for realization of 3D printed phantoms with MEX-AM in CT imaging. For breast imaging, an anthropomorphic phantom with two filaments could be fabricated using ABS-C (conductive acrylonitrile butadiene styrene) as a substitute for breast adipose tissue, and ASA-A (acrylic styrene acrylonitrile) for glandular breast tissue.
Makridis, A., Okkalidis, N., Trygoniaris, D., Kazeli, K., & Angelakeris, M.
Journal of Physics D: Applied Physics, 56(28), 285002
https://doi.org/10.1088/1361-6463/accd01
Three-dimensional (3D) printing technology has emerged as a promising tool for meticulously fabricated scaffolds with high precision and accuracy, resulting in intricately detailed biomimetic 3D structures. Producing magnetic scaffolds with the aid of additive processes, known as 3D printing, reveals multitude and state-of-the-art areas of application such as tissue engineering, bone repair and regeneration, drug delivery and magnetic hyperthermia. A crucial first step is the development of innovative polymeric composite magnetic materials. The current work presents a fabrication protocol of 3D printed polymer-bonded magnets using the Fused Deposition Modeling 3D printing method. Polymer-bonded magnets are defined as composites with permanent-magnet powder embedded in a polymer binder matrix. By using a low-cost mixing extruder, four (4) different filament types of 1.75 mm were fabricated using commercial magnetite magnetic nanoparticles mixed with a pure polylactic acid powder (PLA) and a ferromagnetic PLA (Iron particles included) filaments. The powder mixture of the basic filaments was compounded mixed with the nanoparticles (NPs), and extruded to fabricate the 3D printing filament, which is subsequently characterized structurally and magnetically before the printing process. Magnetic polymer scaffolds are finally printed using composite filaments of different concentration in magnetite. Our results demonstrate that the heating efficiency (expressed in W g−1) of the 3D printed magnetic polymer scaffolds (ranging from 2 to 5.5 W g−1 at magnetic field intensity of 30 mT and field frequency of 365 kHz) can be tuned by choosing either a magnetic or a non-magnetic filament mixed with an amount of magnetite NPs in different concentrations of 10 or 20 wt%. Our work opens up new perspectives for future research, such as the fabrication of complex structures with suitable ferromagnetic custom-made filaments adjusting the mixing of different filaments for the construction of scaffolds aimed at improving the accuracy of magnetic hyperthermia treatment.
Okkalidis, N
Physics in Medicine & Biology, 67(15), 15TR04
https://doi.org/10.1088/1361-6560/ac80e7
Three dimensional (3D) printing technology has been widely evaluated for the fabrication of various anthropomorphic phantoms during the last couple of decades. The demand for such high quality phantoms is constantly rising and gaining an ever-increasing interest. Although, in a short time 3D printing technology provided phantoms with more realistic features when compared to the previous conventional methods, there are still several aspects to be explored. One of these aspects is the further development of the current 3D printing methods and software devoted to radiological applications. The current 3D printing software and methods usually employ 3D models, while the direct association of medical images with the 3D printing process is needed in order to provide results of higher accuracy and closer to the actual tissues’ texture. Another aspect of high importance is the development of suitable printing materials. Ideally, those materials should be able to emulate the entire range of soft and bone tissues, while still matching the human’s anatomy. Five types of 3D printing methods have been mainly investigated so far: (a) solidification of photo-curing materials; (b) deposition of melted plastic materials; (c) printing paper-based phantoms with radiopaque ink; (d) melting or binding plastic powder; and (e) bio-printing. From the first and second category, polymer jetting technology and fused filament fabrication (FFF), also known as fused deposition modelling (FDM), are the most promising technologies for the fulfilment of the requirements of realistic and radiologically equivalent anthropomorphic phantoms. Another interesting approach is the fabrication of radiopaque paper-based phantoms using inkjet printers. Although, this may provide phantoms of high accuracy, the utilized materials during the fabrication process are restricted to inks doped with various contrast materials. A similar condition applies to the polymer jetting technology, which despite being quite fast and very accurate, the utilized materials are restricted to those capable of polymerization. The situation is better for FFF/FDM 3D printers, since various compositions of plastic filaments with external substances can be produced conveniently. Although, the speed and accuracy of this 3D printing method are lower compared to the others, the relatively low-cost, constantly improving resolution, sufficient printing volume and plethora of materials are quite promising for the creation of human size heterogeneous phantoms and their adaptation to the treatment procedures of patients in the current health systems.
Okkalidis, N., Bliznakova, K., & Kolev, N.
Physica Medica, 102, 96-102
https://doi.org/10.1016/j.ejmp.2022.09.009
The aim of this study is the development of a methodology for manufacturing 3D printed anthropomorphic structures, which mimic the X-ray properties of the human bone tissue.
A mixing approach of two different materials is proposed for the fabrication of a radiologically equivalent hip bone for an anthropomorphic abdominal phantom. The materials employed for the phantom were polylactic acid (PLA) and Stonefil, while a custom-made dual motor filament extrusion setup and a custom-made software associating medical images directly with the 3D printing process were employed.
Three phantoms representing the hip bone were 3D printed utilizing two filaments under three different printing scenarios. The phantoms are based on a patient’s abdominal CT scan images. Histograms of CT scans of the printed hip bone phantoms were calculated and compared to the original patient’s hip bone histogram, demonstrating that a constant mixing composition of 30% Stonefil and 70% PLA with 0.0375 extrusion rate per voxel (93.75% flow for fulfilling a single voxel) for the cancellous bone, and using 100% Stonefil with 0.04 extrusion rate per voxel (100% flow) for the cortical bone results in a realistic anatomy replication of the hip bone. Reproduced HU varied between 700 and 800, which are close to those of the hip bone.
The study demonstrated that it is possible to mix two different filaments in real-time during the printing process to obtain phantoms with realistic and radiographically bone tissue equivalent attenuation. The results will be explored for manufacturing a CT-compatible abdominal phantom.
Okkalidis, N., & Bliznakova, K.
Physics in Medicine & Biology, 67(24), 245019
https://doi.org/10.1088/1361-6560/aca640
Objective. In this study, a novel voxel-by-voxel mixing method is presented, according to which two filaments of different material are combined during the three dimensional (3D) printing process. Approach. In our approach, two types of filaments were used for the replication of soft-tissues, a polylactic acid (PLA) filament and a polypropylene (PP) filament. A custom-made software was used, while a series of breast patient CT scan images were directly associated to the 3D printing process. Each phantom´s layer was printed twice, once with the PLA filament and a second time with the PP filament. For each material, the filament extrusion rate was controlled voxel-by-voxel and was based on the Hounsfield units (HU) of the imported CT images. The phantom was scanned at clinical CT, breast tomosynthesis and micro CT facilities, as the major processing was performed on data from the CT. A side by side comparison between patient´s and phantom´s CT slices by means of profile and histogram comparison was accomplished. Further, in case of profile comparison, the Pearson´s coefficients were calculated. Main results. The visual assessment of the distribution of the glandular tissue in the CT slices of the printed breast anatomy showed high degree of radiological similarity to the corresponding patient´s glandular distribution. The profile plots´ comparison showed that the HU of the replicated and original patient soft tissues match adequately. In overall, the Pearson´s coefficients were above 0.91, suggesting a close match of the CT images of the phantom with those of the patient. The overall HU were close in terms of HU ranges. The HU mean, median and standard deviation of the original and the phantom CT slices were −149, −167, ±65 and −121, −130, ±91, respectively. Significance. The results suggest that the proposed methodology is appropriate for manufacturing of anthropomorphic soft tissue phantoms for x-ray imaging and dosimetry purposes, since it may offer an accurate replication of these tissues.
Dukov N, Bliznakova, K, Okkalidis N, Teneva T, Encheva E, & Bliznakov Z.
Physics in Medicine & Biology
https://doi.org/10.1088/1361-6560/ac4c30
Objective. This work describes an approach for producing physical anthropomorphic breast phantoms from clinical patient data using three-dimensional (3D) fused-deposition modelling (FDM) printing. Approach. The source of the anthropomorphic model was a clinical Magnetic Resonance Imaging (MRI) patient image set, which was segmented slice by slice into adipose and glandular tissues, skin and tumour formations; thus obtaining a four component computational breast model. The segmented tissues were mapped to specific Hounsfield Units (HU) values, which were derived from clinical breast Computed Tomography (CT) data. The obtained computational model was used as a template for producing a physical anthropomorphic breast phantom using 3D printing. FDM technology with only one polylactic acid filament was used. The physical breast phantom was scanned at Siemens SOMATOM Definition CT. Quantitative and qualitative evaluation were carried out to assess the clinical realism of CT slices of the physical breast phantom. Main results. The comparison between selected slices from the computational breast phantom and CT slices of the physical breast phantom shows similar visual x-ray appearance of the four breast tissue structures: adipose, glandular, tumour and skin. The results from the task-based evaluation, which involved three radiologists, showed a high degree of realistic clinical radiological appearance of the modelled breast components. Measured HU values of the printed structures are within the range of HU values used in the computational phantom. Moreover, measured physical parameters of the breast phantom, such as weight and linear dimensions, agreed very well with the corresponding ones of the computational breast model. Significance. The presented approach, based on a single FDM material, was found suitable for manufacturing of a physical breast phantom, which mimics well the 3D spatial distribution of the different breast tissues and their x-ray absorption properties. As such, it could be successfully exploited in advanced x-ray breast imaging research applications.
Okkalidis, N., & Marinakis, G.
Medical Physics, 47(5), 2206-2211
https://doi.org/10.1002/mp.14100
The fabrication of a realistic patient-specific skull phantom employing for the first time a new filament extrusion rate method, for the accurate replication of soft and bone tissues both in Hounsfield Units (HU) range and in texture.
An in-house developed software was used for the fabrication of the phantom taking into account all the HU of a patient’s Computed Tomography (CT) images, replicating the organs voxel-by-voxel without the need of a uniform three-dimensional printing pattern. Two commercially available materials were used; the polylactic acid (PLA) filament for the soft tissues, and a mixture of 50% of PLA and 50% of gravimetric powdered stone for the bone tissues. Additionally, a layer of small amounts of PLA were also extruded on the fabricated bones.
The replicated anatomy of the phantom was very close to the patient’s one, achieving a similar range of HU without creating any air gaps and variations on the replicated HU, which are the main artifacts observed when a standard infill density and pattern is employed. The maximum measured HU values of the replicated bone tissues were at about 900.
The results indicated an accurate replication of the soft tissues HU, and a significant improvement of the bone tissue HU replication. Further investigation on materials of high density in conjunction with the filament extrusion rate method may provide custom-made realistic phantoms for diagnostic and lower energy radiation such as in superficial, orthovoltage, and electron beam radiotherapy.
Okkalidis, N.
Medical Physics, 45(10), 4600-4606
https://doi.org/10.1002/mp.13154
A novel 3D printing method has been developed, which employs human CT images to construct patient specific phantoms by controlling the filament extrusion rate.
An in-house software was developed comprising pixel-by-pixel (PbP) reading of the Hounsfield Units (HU) values in the original patient DICOM images and their sufficiently accurate 3D printed replication in the phantom produced.
The PbP method was applied to two sets of anonymized patients’ CT chest and skull images. The respective patient specific phantoms were 3D printed and then CT scanned and compared to the actual patient images. The chest phantom images were also compared to those of another phantom created employing the older variable infill density method (VID).
The results clearly indicated a significant improvement both visually and in the phantom HU values achieved. In contrast to other methods published, its major advantages are: (a) no need for manual contouring and 3D modeling of a patient’s organs, (b) wider density range, and (c) significantly better simulation of the organs’ HU.
Okkalidis, N., Chatzigeorgiou, C., & Okkalides, D.
Journal of Engineering and Science in Medical Diagnostics and Therapy
https://doi.org/10.1115/1.4038228
A couple of fused deposition modeling (FDM) three-dimensional (3D) printers using variable infill density patterns were employed to simulate human muscle, fat, and lung tissue as it is represented by Hounsfield units (HUs) in computer tomography (CT) scans. Eleven different commercial plastic filaments were assessed by measuring their mean HU on CT images of small cubes printed with different patterns. The HU values were proportional to the mean effective density of the cubes. Polylactic acid (PLA) filaments were chosen. They had good printing characteristics and acceptable HU. Such filaments obtained from two different vendors were then tested by printing two sets of cubes comprising 10 and 6 cubes with 100% to 20% and 100% to 50% infill densities, respectively. They were printed with different printing patterns named “Regular” and “Bricks,” respectively. It was found that the HU values measured on the CT images of the 3D-printed cubes were proportional to the infill density with slight differences between vendors and printers. The Regular pattern with infill densities of about 30%, 90%, and 100% were found to produce HUs equivalent to lung, fat, and muscle. This was confirmed with histograms of the respective region of interest (ROI). The assessment of popular 3D-printing materials resulted in the choice of PLA, which together with the proposed technique was found suitable for the adequate simulation of the muscle, fat, and lung HU in printed patient-specific phantoms.
We would like to thank again all our partners for joining and contributing to MORPHE workshop’s success! Your support and collaboration is truly appreciated. We look forward to future opportunities …
Morphé has joined the Action “Elevating Greek Startups against COVID 19 2nd CYCLE”. The Action aims at the support of start-ups included in the National Register of Start-ups “Elevate Greece” in …
The past year, Morphé and partners were accepted for a Horizon 2020 Marie Curie RISE funding program for the development of anthropomorphic breast phantoms implementing our 3D printing technology.
Morphé was chosen to participate to ‘Ok!Thess’ accelerator for further market research and development of its services.







